Product Release Version: v25.3.0
January 2025 Product Release
© 2025 Practice Management System
Disclaimer: All rights are reserved. No part of this work may be reproduced in any form or by any means graphic, electronic, or mechanical, including photocopy, recording, or information storage and retrieval systems – without written permission of the publisher.
The products that are referred to in this document may be either trademarks and/or registered trademarks of the respective owners. The publisher and the author do not claim these trademarks.
While every precaution has been taken in the preparation of this document, the publisher and the author assume no responsibility for errors or omissions or for damages resulting from the use of the information contained in this document or from the use of programs and source code that may accompany it. In no event shall the publisher and the author be liable for any loss of profit or any other commercial damage caused or alleged to have been caused directly or indirectly by this document.
Printed January 2025 at PracticeSuite, Inc.
Part 1- Product Enhancements
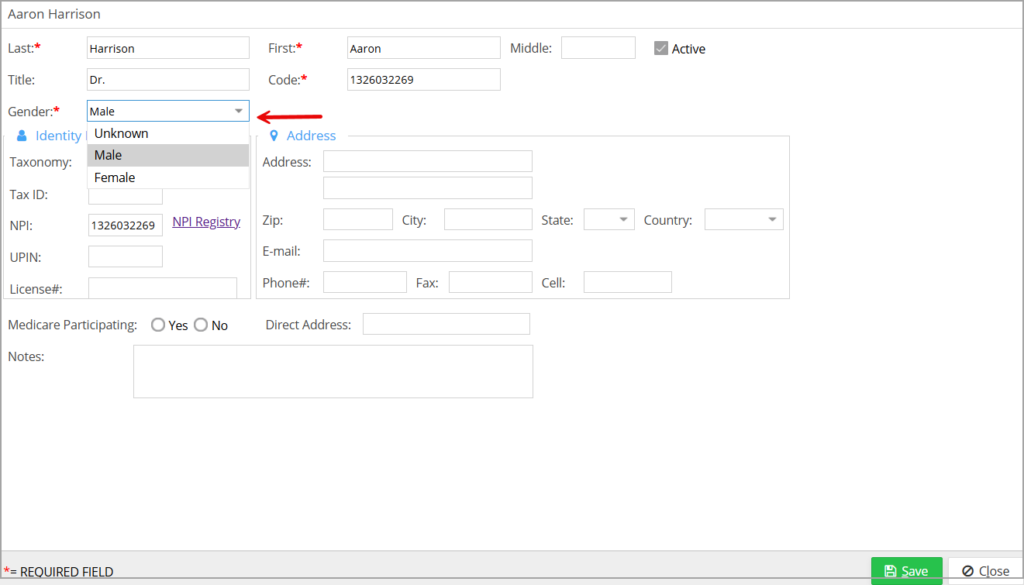
1.11 Referring Provider Master- Gender Field Update
A dropdown is added to select the gender in the Referring Provider Master screen (Image 1.11).
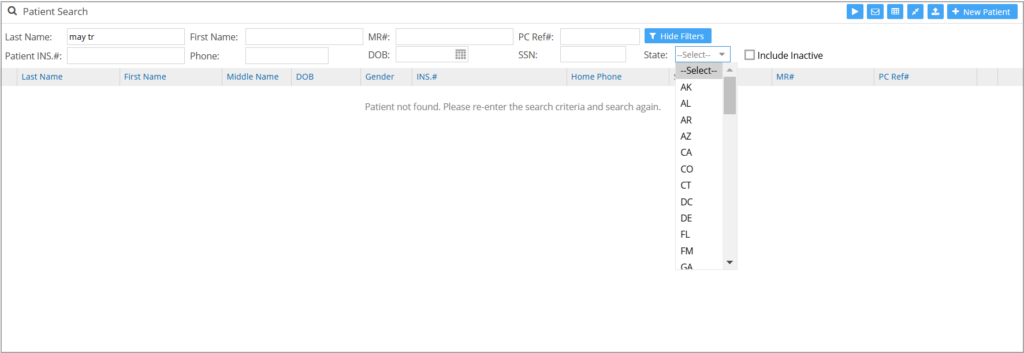
1.12 Patient Search Screen Update
A filter to search by State has been added to the patient search screen. Please see Image 1.12.
1.13 Document Manager –Default ‘Share with Patient’
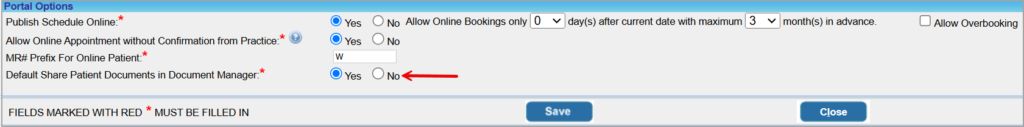
To make it easier to share documents with patients via the Hello Health patient engagement portal, the option ‘Share with Patient’ checkbox in the Document Manager can be defaulted to ‘Yes’. Previously, users had to individually select the option for the document even if most of them had to be shared.
To enable the default to ‘Yes’, a setting has been added to the Portal Options page named Default Share Patient Documents in Document Manager, and selecting ‘Yes’ will automatically select the ‘Share with Patient’ checkbox. Please see Image 1.13.
1.14 Patient Portal – Quick Pay Screen
The Patient Portal Quick Pay screen now allows flexible entry of statement # and supports inputs with or without hyphens, spaces, or case sensitivity. This enhancement simplifies the process, minimizing input errors, and improving user experience.
1.15 Letter Master- Added New Tags
The following tags have been added to the Letter Master and will be available in Scheduler and Patient Master.
#@Provider FName#@ #@Provider MName#@ #@Provider LName#@
Reports
1.16 Update to ‘I22. Charges and Payments by Referring Physicians Report’
The ‘I22. Charges and Payments by Referring Physicians Report’ has been updated to align with the system’s month-end close processes and reporting prerequisites.
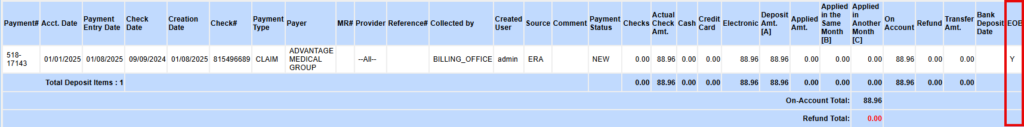
1.17 I4 Report – EOB Flag
The ‘I4. Payment Deposit Report’ now includes an EOB flag to indicate if an EOB file was uploaded to the payment entry. ‘Y’ in the column is indicative that the EoB was uploaded, while ‘N’ indicates otherwise.
1.18 J22 Report – LE Address on Header
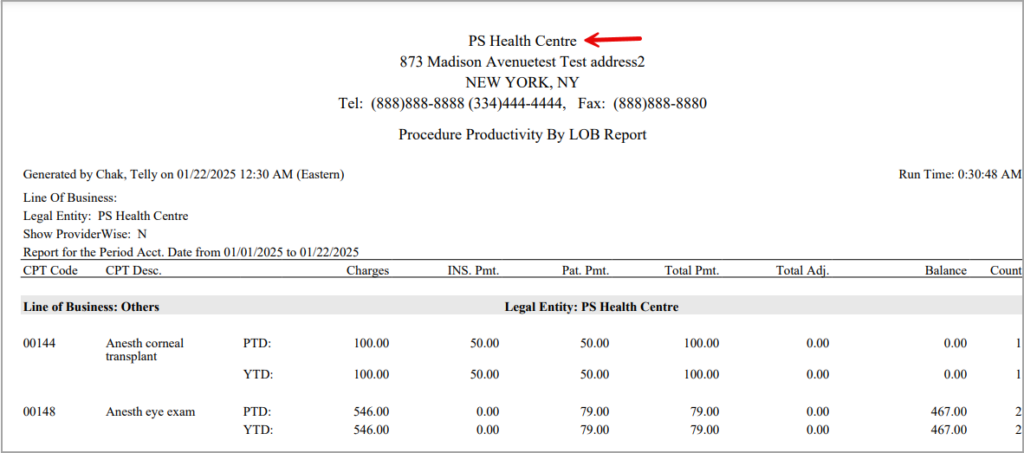
The ‘J22. Procedure Productivity by LOB Report’ will display the address of the Legal Entity in the header if the user has selected an LE when running the report. The patient ledger PDF header will also display the same LE address. Please refer to Image 1.18.
On the other hand, if ‘All’ is selected in the LE filter, then the header will display the primary address of the Legal Entity.
1.19 I5 Report – Added Patient’s Address
‘I5. The On Account Payment Report’ will include the patient’s full address on the on-screen display and the Excel export.
Part 2: Resolved Items
Practice Management
2.1 ERA
2.1.1 Partial Refunds Error
An issue with partial refunds in the PLB section of the ERA where refunds were not working correctly when matched with the claim# has been resolved. Users can now successfully process partial refunds by matching the claim number or the payment number.
2.2 Claims Workbench Performance
The performance issue with the Claims Workbench has been resolved.
2.3 Denials in Collections Manager
When a previously worked claim reappears in the Collection Manager after a new denial is posted, it will fall into the ‘New’ list instead of the existing status list.
2.4 Case Switch – Line Status
When switching a case for an encounter billed to a secondary or tertiary payer, if the target case does not have a secondary or tertiary payer, the line status will revert to the status before it was billed to the secondary.
2.5 XSuperbill Processing
Previously, even if the claim rule validation was not enabled for an account, the check box beside the claim on the XSuperbill screen remained unavailable, stopping the claims from being processed. This issue has been resolved.
2.6 Manual Payment Posting
The issue preventing users from posting payments after clicking the reverse button on the manual posting screen has been resolved.
General
2.7 Security- Certain Screens Unavailable for 2FA-Enabled Users
2FA-enabled users encountered the login page upon attempting to access the Patient Master or the Case Screen from the Charge Master. A hotfix was released to resolve this issue.
2.8 Group Login- Patient Master and Insurance
When accessed from the single sign-on login screen, the patient demographics screen was grayed out and the insurance area displayed no information. Both the issues were resolved in a hotfix release.
Reports
2.9 D2 Report – Aging Summary and Aging Buckets
In ‘D2. Detailed-Insurance Aging Report’, there was a mismatch in the amounts shown in the aging summary and the buckets. This discrepancy has been corrected.
2.10 D3 and D6 Mismatch
The discrepancy between the ‘D3. Summary- Patient/Guarantor Balance and Aging Report’ and ‘D6. A/R Aging Summary Report’ has been resolved.
2.11 D4 Report- Last Payment Date Error
The ‘Last Patient Payment Date’ column in the ‘D4. Summary- Insurance Balance and Aging by Patient Report’ erroneously displayed the auto-adjustment date if it was the last activity present for the line. This issue has been corrected.